
Specific Social and cultural norms determine the style of parenting but the core parental function of meeting the child's needs is universal.
Parental Mental Health and Child Welfare
This page aims to facilitate an understanding of the processes that underlye and influence how parental mental illness can affect children, can affect the parent-child relationship, how parenthood can preciptate and influence mental illness and how a child's mental health and development needs can have an impact on parental mental health.
To meet a child's needs, parents should be able to provide a safe physical environment, provide a secure emotional environment, enabel and give appropriate opportunities for the child's development, model appropriate behaviour, show an interest in and approval of their child and their achievements.
Depression, substance dependence, and personality disorder occurring together in various combinations at various points in time are the most frequently reported psychiatric conditions affecting parents who maltreat their children. Parents (and their partners) who experience a combination of personality disorder, substance dependence, other mental illness, and violent or discordant relationships are least able to meet their children's needs and represent the greatest risk to their safety and future development.
It is important of course to note that the majority of mentally ill parents do not abuse or maltreat their children.
Moreover, individual risk factors and stressors tend to be insufficient on their own as causes of serious inability to provide effective parenting; it is the combination of personality factors, coping skills, social supports and factors within the child as well as the presence of mental illness in a parent, that in aggregate determine whether or not abuse and maltreatment will occur.
Facts and Figures
|
1 |
All adults have a one in four chance of experienceing a period of mental illness during their lifetime. This includes a wide range of mental ill health, from mild to severe, and from single episodes to chronic conditions. |
|
2 |
5.7 million adults (12.6% of the adult population) are suffering from a mental illness at any one time. |
|
3 |
30% of mentally ill adults will have dependent children (0-10 years old). |
|
4 |
3.8% of all parents with dependent children have a mental illness (this amounts to about 1.7. million adults and 2.5 million children). |
|
5 |
Approximately 10 000 children and young people are caring for a mentally ill parent. |
|
6 |
33% to 66% of children who have a mentally ill parent are adversely affected. A conservative estimate is that one-third of children living with a mentally ill parent will themselves develop significant psychological problems or disorders. A further third will develop less severe emotional and behavioural difficulties, which may nevertheless be significant for their longer term development. |
|
7 |
1.4 million children (12% of the total child population of 11.6 million) will experience an emotional and behavioural disorder during childhood. |
|
8 |
33% of children with emotional and behavioural disorders have a parent with a mental health problem. |
|
9 |
One-third to three-quaters of parents whose children are known to children's services experience mental health problems. More than one-third of mothers of children on social work caseloads were found to be moderately to severely depressed . At least 25% of children who are the subject of child protection conferences have a parent with mental health problems. Parental mental health is an important factor in children becoming looked after by local authorities. |
|
10 |
One in 10 people with a psychotic illness attempt to commit suicide |
Key Features of Adult Mental Illness
|
Depression |
Core symptoms: Depressed mood; loss of interest and enjoyment; reduced energy, tiredness and diminished activity Supplementary Symptoms: Reduced concentration and attention; reduced self esteem and self confidence; suicidal or self-harming ideation; disturbed sleep (initial insomnia, early waking and broken sleep); loss of appetite and weight |
|
Bipolar Affective Disorder |
Depressive Symptoms (See Depression above) and more likely to have symptoms of: loss of appetite and weight; difficulty in getting to sleep; constipation; loss of libido. Manic Symptoms Include: Being extremely happy and excited (euphoric); irritation with those who do not share the same optimistic outlook; being full of energy; unable or unwilling to sleep; feeling full of new and exciting ideas; feeling more important than usual; hearing voices Other possible symptoms include: Jumping from idea to idea; making grandiose and unrealistic plans; moving very quickly and being very active; behaving in a bizarre way; speaking very quickly; making odd and impulsive decisions; reckless spending of money; sexual disinhibition |
|
Anxiety |
Symptoms of the Mind include: Feeling worried all of the time; feeling tired; inability to concentrate; feeling irritable; sleeping badly Symptoms of the Body include: irregualr heartbeat; sweating; muscle tension and pains; breathing heavily; dizziness; feeling faint; indigestion; diahorrea |
|
Schizophrenia |
A disconnection of thoughts, feelings and action Poitive Symptoms: Hallucinations; Delusions Negative symptoms - Absence of normal behaviour: apathy; lack of energy and interest in life; lack of emotions and "get up and go"; interference of speecjh or behaviour; lack of motivation; withdrawal; self neglect; blunted emotions |
|
Personality Disorder |
A Pattern of Behaviour: Emotional response; perception of self, others and the environment Which is: Evident in early life, persists into adulthood, pervasive, inflexible, a deviation from the person's cultural norm and Leads To: Distress to self; others, or society; dysfunction in interpersonal, social or working relationships Symptoms May Include: Hostile behaviour towards others, irritability; difficulty relating to others in a constructive way; inability to separate own needs from those of others; alcohol and substance misuse; anxiety and depression; deliberate self harm; bingeing, vomiting, purging and other eating problems |
People from ethnic minorities often experience inequalities in health and healthcare.
Insufficient knowledge and awareness of other cultural beiliefs and practices in relation to mental illness can lead to errors in assessment, diagnosis, and care planning together with inappropriate management and poor compliance.
Evidence from transcultutral studies have shown that major mental illnesses such as schizophrenia and depressive illnesses occur worldwide but culture will determine the content of the symptoms and how they are expressed. Delusions and halucinations are based upon the symbols and images of the individual's cultural milieu.
In the past 30-40 years there have been significant changes in family structures and women's roles. Two changes affecting women and their mental health are the increase in lone parents and the growing number of women who are returning to the workforce who have children and may be parenting alone. These changes have important implications for those who provide services because meeting women's various needs requires different, flexible approaches e.g women with young children are at particular risk for developing depression.
The increasing number of women entering the workforce therefore effects many who are also mothers. The nature of the employment (quality, remuneration, pattern) is an important determinant of mental health e.g. part time work appears to have a protective effect whilst studies suggest that mothers in full-time employment who have responsibility for young children are at particular risk.
Links between mental health and violence in families are complex: few studies have systematically explored the combination of family violence involving both dependent children and their mentally ill parents.
There are few studies that have reported associations between the presence of specific mental illness and violence within families with dependent children but more research is required to determine causal links and mechanisms.
Studies of mothers in families where physical abuse of children has occurred have found associations with low income, youthful parenthood, less education, histories of abuse in their childhood, and alcohol or drug dependence.
Other studies have noted the combination of personality disorder and substance misuse in parents who have been both victimss of violence (e.g. by a partner) and perpetrators (maltreatment of their children).
Excessive alcohol consumption is an important accompaniment to violence in families and associated abuse and neglect of children, together with children being "looked after". Bland and Orn have found that alcoholism combined with anti-social personality and/or depression produced significantly high rates of violence within families. They also found that parents who made previous suicide attempts were more likely to exhibit violent behaviour.
The Family Model: A Systemic Conceptual Model for exploring the key components of the links between child and adult mental health
The links between poverty, mental ill health, discrimination and social exclusion are compelling. Any attempt to improve the life chances for mentally ill parents and for their children must be based on a good understanding of child and parent within the family context. This includes parents or caregivers and the wider family, as well as neighbourhood, community and cultural influences.
The combination of ethnic minority status and female gender (and associated gender based discrimination), coupled with parental responsibilities (which are disproportionately placed with women), enhances the risks for the onset and/or exacerbation of mental illness which, in turn, compounds the experience of discrimination and social exclusion for all family members
There is an emphasis on maternal mental health in the literature concerning parental mental health. Less work has been done with regard to fathers and male gender in general.
Promoting positive mental health across the life span and between generations requires broader approaches to assessment and intervention, incorporation of a perspective on prevention into daily practice and good collaboration between all children and families services, mental health services and a wide range of other agencies.
RESOURCE: For a comprehensive review of Fatherhood and Mental Health visit the Australian Institute of Family Studies publications page Here
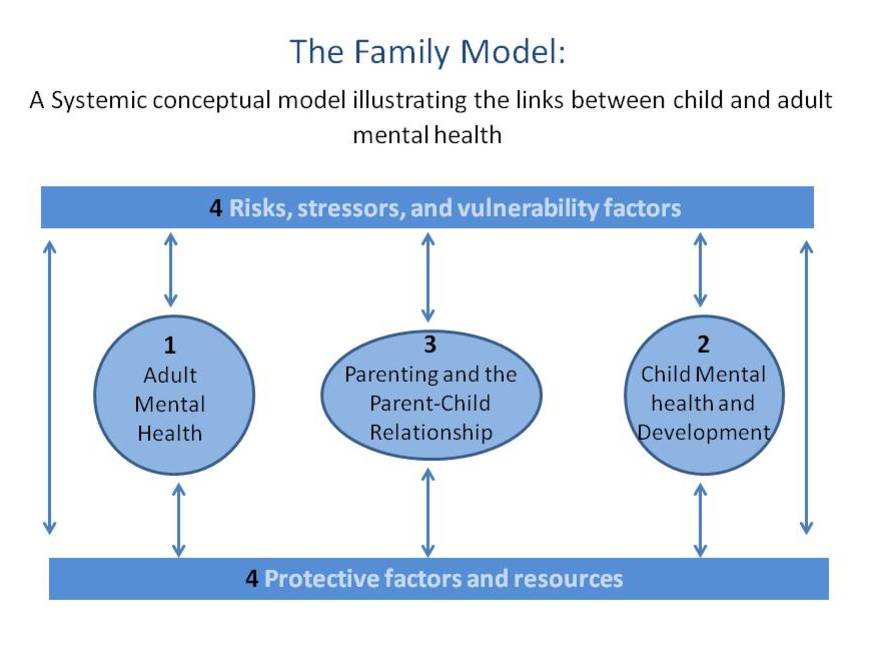
An integrated, ecological model of influences and interactions between mental illness, parenting, family relationships, child development and environmental risk factors and protectors was developed in Crossing Bridges – training materials, sponsored by the Department of Health, on the impact of parental mental illness on children (Falkov, 1998).
This model emphasises the relevance of a systems approach to assessment and intervention. Each component affects, and is affected by, every other component. Such an approach requires consideration of:
The tasks and responsibilities of parenthood and an individual’s coping resources (including family of origin and childhood experiences as well as susceptibility to difficulties in the transition to parenthood)
Unique aspects of the relationship between a parent and child
The nature of the mental illness experienced by the adult




